The ABCs of hCG

If you’ve heard of hCG (which stands for human chorionic gonadotropin) but you don’t quite know why it’s so important, you’re not alone. Here we explore hCG and its key role in detecting pregnancy. In some cases, your doctor may ask to do blood draws to look for changes in your hCG levels, highlighting just one of the reasons it’s important to establish a good relationship with an ob-gyn early in your pregnancy.
What is hCG?
Home pregnancy tests can detect hCG, a hormone first made by the embryo and then by the placenta. It appears first in blood and then in your urine,1 so your healthcare provider can also detect hCG using a blood test. Clearblue® Early Detection Pregnancy Test provides early detection of the pregnancy hormone (hCG) in urine. 71% of pregnancies can be detected 6 days before the missed period (5 days before the expected period).
What does hCG do?
The hCG hormone is impressive. Its main role is to help your body maintain high levels of the hormone progesterone to support your uterine lining. The production of progesterone prevents menstruation (the breakdown and shedding of the uterine lining) and the start of a new cycle.2 Throughout pregnancy, hCG also promotes the formation of new blood vessels in the uterus, protects the placenta from foreign cells, helps the uterus grow, helps suppress Braxton Hicks contractions, and promotes growth of the umbilical cord and fetal organs.3
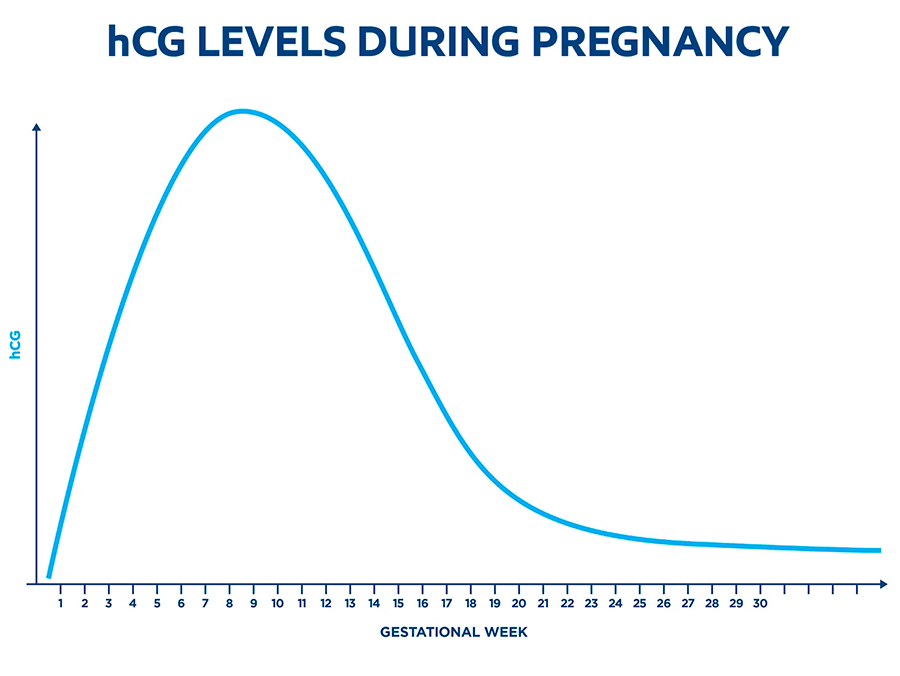
It’s important to know that even in normal pregnancies, hCG levels vary greatly from person to person. Typically, the levels of hCG double about every two days during the first 10 weeks, peak at around week 10, slowly decline, and then remain stable until the baby is born.4
Why do some women need to have their hCG levels monitored?
Home pregnancy tests are qualitative, which means they simply tell you if the hCG hormone is present in your urine or not. Monitoring hCG levels is a way of gathering information about the status of the pregnancy. If your doctor wants to monitor your hCG levels, you’ll need a quantitative test, which measures the amount of hCG in your blood. Most U.S doctors only monitor the hCG levels if you have a history of miscarriage or ectopic pregnancy, or if you’re showing symptoms of a possible early pregnancy loss.
Monitoring hCG levels often requires two or more blood draws, typically 48 to 72 hours apart. Remember: The average levels of hCG can vary greatly. It’s not necessarily the number that’s most important, but whether the number is changing. HCG levels can also vary in multiple pregnancies (for example, if you’re having twins).
Don’t use home pregnancy tests to try to track your hCG levels, as they are not designed for this purpose. Different home pregnancy tests have different sensitivity levels, and results can also be dependent on other factors such as whether or not you used early morning urine.
If your hCG levels are low, you could have miscalculated the expected date of your period. HCG levels that don’t rise as expected could indicate an early pregnancy loss (including ectopic pregnancy and miscarriage); additional hCG tests or an ultrasound performed by your doctor can confirm this.6
If your hCG levels are high, you may simply be further along in your pregnancy than you originally thought. You may have also heard that high levels of hCG mean you’re having multiples. This is not entirely true. Because individual hCG levels vary greatly, a multiple pregnancy can only be confirmed by ultrasound.7 High levels of hCG could also indicate a rare condition called a molar pregnancy. If you have symptoms such as vaginal bleeding, pelvic pressure or pain, severe nausea or vomiting, or anything else you’re concerned about, see your doctor.8
Are there standard amounts of hCG by week?
No, and hCG levels vary so much week by week that hCG level charts generally aren’t helpful. In most pregnancies, what matters most is the presence of hCG, which can be detected using a home pregnancy test. Home pregnancy tests can’t check the exact levels of hCG.
Perhaps you’re reading this because your doctor wants to check your hCG levels, and you’re worried. That’s normal. Just remember that it often takes two (or more) tests to know what’s happening. It may help to bring your partner, a family member or friend with you to the blood draws, and to any appointments where you may learn the results. And know this: When a healthcare professional notes that they’re drawing blood to measure your hCG levels, they’re often incredibly kind. Many women just like you have shakily sat in their chair and have experienced the same set of tests. While you wait for the result, or through the long 48 to 72 hours before the next draw, check out stories from #Conceivinghood and know you’re not alone.

Looking for insights on your health journey? Clearblue® sends you curated, science-backed articles right to your inbox.
Sources and disclaimers
- Betz D, Fane K, “Human Chorionic Gonadotropin,” August 11, 2021, StatPearls, https://www.ncbi.nlm.nih.gov/books/NBK532950/.
- Pregnancy Calendar: A week-by-week guide, (n.d.). KidsHealth from Nemours, https://kidshealth.org/en/parents/week4.html.
- “Changes During Pregnancy,” (October 2020), The American College of Obstetricians and Gynecologists, https://www.acog.org/womens-health/infographics/changes-during-pregnancy
- Gnoth, C., & Johnson, S, (July, 2014), “Strips of hope: accuracy of home pregnancy tests and new developments,” Geburtshilfe und Frauenheilkunde, 74(07), 661-669, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4119102/
- “What is HCG?” (n.d.), American Pregnancy Association, https://americanpregnancy.org/getting-pregnant/hcg-levels/
- “Early Pregnancy Loss,” (February 2020), The American College of Obstetricians and Gynecologists, https://www.acog.org/womens-health/faqs/early-pregnancy-loss
- Seeber BE, (November 2012), “What serial hCG can tell you, and cannot tell you, about an early pregnancy,” Fertility and Sterility, 8(5), https://www.fertstert.org/article/S0015-0282(12)02233-9/pdf
- SCavaliere A., Ermito S., Dinatale A., & Pedata R, (2009), “Management of molar pregnancy,” Journal of Prenatal Medicine, 3(1), 15–17, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3279094/

What are the early signs of pregnancy?
There are various symptoms that can indicate you might be pregnant, even if you might not experience any/all of them.




